Facts About Monkeypox: Signs, Symptoms, Treatment and Vaccines
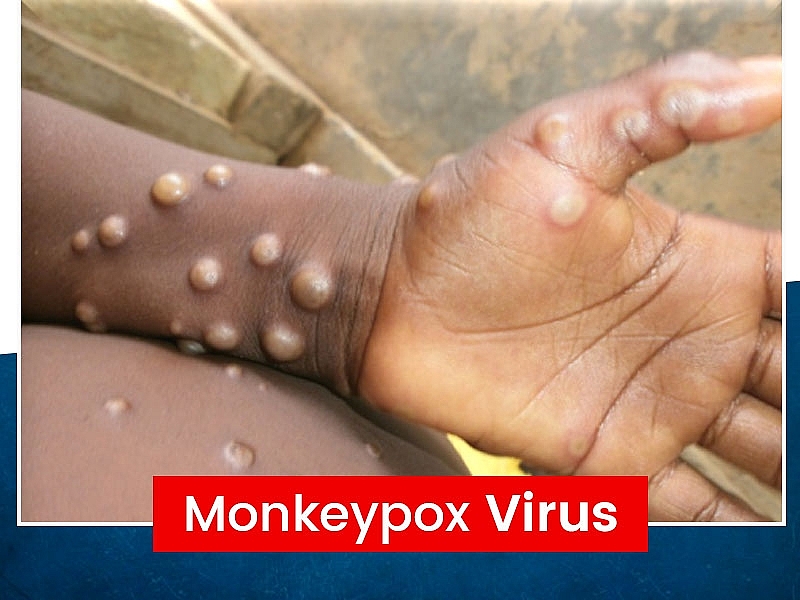 |
| Find out the monkeypox cases around the world right now |
Monkeypox Key Facts
♦ Monkeypox is a rare disease that occurs primarily in the rainforest countries of Central and West Africa.
♦ Monkeypox is a viral disease that produces pox-like lesions on the skin. It is closely related to smallpox but is not nearly as deadly as smallpox was.
♦ Monkeypox is similar to smallpox, and the monkeypox virus causes monkeypox.
♦ The history of monkeypox is new (1958), and medical professionals diagnosed the first human monkeypox cases and differentiated them from smallpox in the early 1970s.
♦ Health researchers have identified the viral infection in laboratory monkeys, African tree squirrels, mice, rats, and rabbits.
♦ Monkeypox can spread to humans. Early symptoms include fever, headache, muscle aches, backache, swollen lymph nodes, a general feeling of discomfort, and exhaustion.
♦ Monkeypox virus is transmitted from one person to another by close contact with lesions, body fluids, respiratory droplets and contaminated materials such as bedding.
♦ Later symptoms occur one to three days or more after the appearance of fever and include a rash with raised bumps, often first developing on the face. During the first few days, symptoms are nonspecific and include fever, nausea, and malaise. After about four to seven days, lesions (fluid-filled pustules, papules) develop on the face and trunk that ulcerate, crust over, and begin to clear up after about 14-21 days, and lymph nodes enlarge. There may be some scarring.
♦ Monkeypox can spread to humans from an infected animal through an animal bite or direct contact with the animal's lesions or bodily fluids.
♦ The disease can spread from person to person, although it is not as contagious as smallpox.
♦ Monkeypox can be fatal in up to 10% of cases.
♦ Monkeypox is preventable as long as people avoid direct contact with infected animals and people. Vaccination against smallpox seems to afford about an 85% chance of avoiding the infection.
♦ There is currently no available treatment for monkeypox.
♦ There is no commercially available vaccine specifically for monkeypox. Vaccines used during the smallpox eradication programme also provided protection against monkeypox. Newer vaccines have been developed of which one has been approved for prevention of monkeypox
♦ Research is ongoing to study antivirals, genetics, and rapid tests for monkeypox.
♦ Treatment may consist of immediate vaccination with smallpox vaccine because monkeypox is so closely related to smallpox and thus cross-protective. Treatment with an antiviral drug or human immune globulin has been done.
♦ Health agencies have said that most of the cases were detected in gay men.
| The name “monkeypox” comes from the first documented cases of the illness in animals in 1958, when two outbreaks occurred in monkeys kept for research. However, the virus did not jump from monkeys to humans, nor are monkeys major carriers of the disease. |
Monkeypox Virus Outbreak - Latest Cases Around the World
► The European Union's disease agency that the number of monkeypox cases has reached 219 outside of countries where the virus usually circulates. The World Health Organisation has warned of more cases in coming days
The UK reported its first monkeypox case in early May. Since then, the virus has spread rapidly in the country with the infection count now at 90.
Spain has reported 98 confirmed cases of monkeypox so far.
Portugal has meanwhile registered 74 confirmed cases, health authorities said Friday, adding that all the occurrences are in men, mainly aged below 40.
The World Health Organization has cautioned that the 200 monkeypox cases found in recent weeks outside of countries where it is an endemic could be just the beginning.
► Monkeypox is primarily spreading through sex:
While the virus itself is not a sexually transmitted infection, which are generally spread through semen and vaginal fluids, the most recent surge in cases appears to have been spread among men who have sex with other men, WHO officials said, emphasizing that anyone can contract monkeypox.
► Monkeypox is spreading around the world last days. There's a monkeypox outbreak in the United Kingdom, Portugal, Spain and other European countries.
In outbreak of the monkeypox virus in North America and Europe is primarily spreading through sex among men with about 200 confirmed and suspected cases across at least a dozen countries.
Individuals exhibiting symptoms of the virus — which include rashes and fever — are being urged to seek medical advice, contacting any clinic before visiting.
In the U.K. alone, cases have doubled since the first was identified on May 7. The country now has 20 confirmed cases, though concerns are building that more may be going undetected.
The U.S. comfirmed its first monkeypox case of the year on Wednesday — a man in Massachusetts — followed by a second on Friday in New York City.
Australia reported one case Friday, in a traveler who recently returned from Britain.
Most of those countries have more suspected cases awaiting confirmation.
Health authorities in Europe, the U.S. and Australia are investigating a recent outbreak of monkeypox cases, a rare viral disease typically found in Africa.
U.S. CDC Guidelines on Monkeypox VaccineThe Jynneos vaccine, made by Bavarian Nordic will be available for certain healthcare workers and laboratory personnel at a time when monkeypox infections has spread in Europe, United States and beyond. The vaccine was approved in the United States in 2019 to prevent smallpox and monkeypox in high risk adults aged 18 and older. CDC officials earlier this week said they were in the process of releasing some doses of the Jynneos vaccine for people in contact with known monkeypox patients. Officials said there were over 100 million doses of an older smallpox vaccine called ACAM2000, made by Emergent BioSolutions which has significant side effects. |
What is Monkeypox and How Dangerous is It?
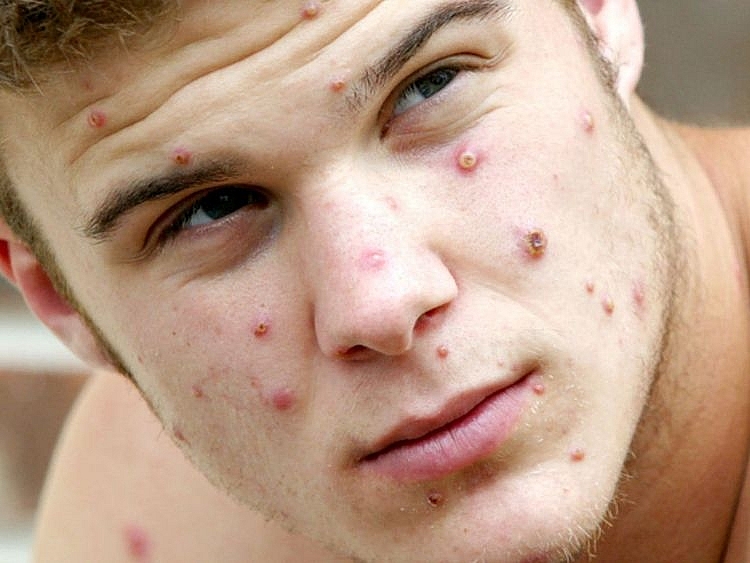 |
| High school student Julian Glenn was believed to have contracted the monkeypox virus from his pet prairie dog, John, in this file photo taken in 2003. |
Monkeypox is a rare disease caused by the monkeypox virus, part of the same family as smallpox, though typically less severe.
Generally occurring in remote parts of Central and West Africa, the virus was first detected in captive monkeys in 1958.
Monkeypox was first identified in 1958 in monkeys in the Democratic Republic of Congo. It wasn't until 12 years later, in 1970, that the first human cases were identified.
The first human case was recorded in 1970.
There have since been sporadic cases reported across 10 African countries, including Nigeria, which in 2017 experienced the largest documented outbreak, with 172 suspected and 61 confirmed cases. Three-quarters were among males aged 21 to 40 years old.
Cases outside of Africa have historically been less common, and typically linked to international travel or imported animals. Previous cases have been reported in Israel, the U.K., Singapore and the U.S., which, in 2003, reported 81 cases linked to prairie dogs infected by imported animals.
It causes less severe disease than smallpox, but monkeypox infections still are serious.
There are two known types. The West African clade is estimated to be fatal in 1 in 100 people, but an infection with the Congo Basin clade is deadlier. Its mortality rate is about 1 in 10, according to the World Health Organization.
The virus is more likely to be fatal in young children.
How dangerous is it?
Monkeypox cases can occasionally be more severe, with some deaths having been reported in West Africa.
However, health authorities stress that we are not on the brink of a serious outbreak and the risks to the general public remain very low.
“While investigations remain ongoing to determine the source of infection, it is important to emphasize it does not spread easily between people and requires close personal contact with an infected symptomatic person,” Colin Brown, director of clinical and emerging infections at the UKHSA, said Saturday.
Health authorities in the U.K., U.S. and Canada urged people who experience new rashes or are concerned about monkeypox to contact their health-care provider.
The UKHSA added that it is reaching out and providing advice to any potential close contacts of cases and health-care worker who may have come into contact with infected patients.
| Is monkeypox fatal? Monkeypox is milder than smallpox, but it can still be fatal. Monkeypox causes death in up to 10% of cases. The case fatality ratio of monkeypox has historically ranged from 0 to 11 % in the general population and has been higher among young children. In recent times, the case fatality ratio has been around 3-6%, according to WHO. A note from Cleveland Clinic: Monkeypox is a rare disease similar to smallpox. It occurs mainly in western and central regions of Africa and usually isn’t a cause for concern in the United States. However, outbreaks have occurred, and it’s important to be aware of the symptoms. Early symptoms are flu-like and include fever, chills and body aches. After a few days, a rash will begin to develop. Monkeypox is milder than smallpox, but it’s still important to be seen by a healthcare provider if you develop any symptoms. |
Symptoms and Signs of the Monkeypox Virus
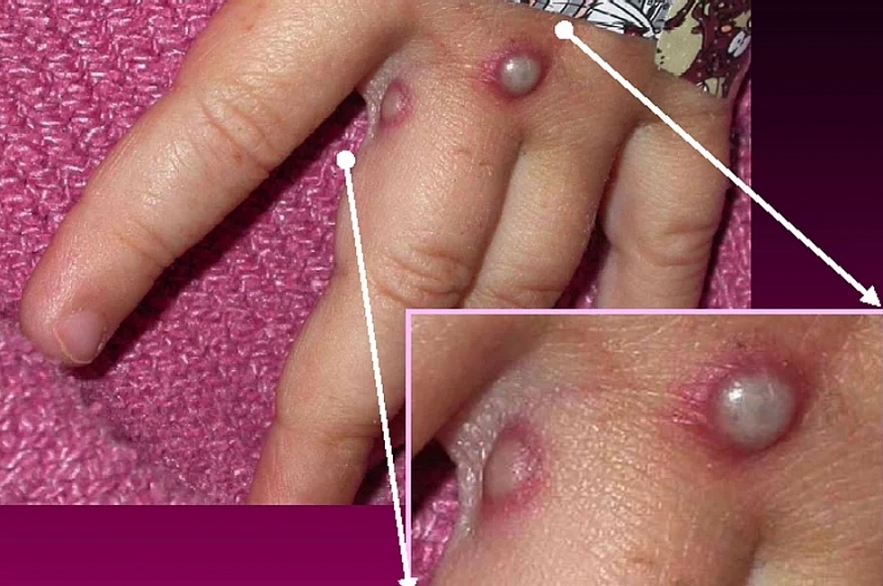 |
| Symptoms of the monkeypox virus |
Initial symptoms of monkeypox include fever, headaches, muscle ache, swelling and backpain.
Symptoms of the monkeypox virus are shown on a patient's hand, from a 2003 case in the United States. In most instances, the disease causes fever and painful, pus-filled blisters. New cases in the United Kingdom, Spain and Portugal are spreading possibly through sexual contact, which had not previously been linked to monkeypox transmission.
It can take up to 21 days for symptoms to develop after a person is infected, according to the CDC. But when symptoms appear, they are typically flu-like and include swelling of the lymph nodes. Common are:
→ Fever
→ Headache
→ Muscle aches
→ Backache
→ Swollen lymph nodes
→ Chills
→ Exhaustion
From one to three days after the flu-like symptoms begin, people typically develop a rash and lesions that may start in one place on the body and spread to other parts.
Lesions progress through stages and scab before falling off.
The illness typically lasts two to four weeks, and could initially be confused with a sexually transmitted disease such as syphilis or herpes.
Patients typically develop a rash one to three days after the appearance of fever, often beginning on the face and spreading to other parts of the body, such as the palms of the hands and soles of the feet.
The rash, which can cause severe itching, then goes through several stages before the legions scab and fall off.
According to WHO, the infection can be divided into two periods:
► the invasion period (lasts between 0-5 days) characterized by fever, intense headache, lymphadenopathy (swelling of the lymph nodes), back pain, myalgia (muscle aches) and intense asthenia (lack of energy). Lymphadenopathy is a distinctive feature of monkeypox compared to other diseases that may initially appear similar (chickenpox, measles, smallpox)
► the skin eruption usually begins within 1-3 days of appearance of fever. The rash tends to be more concentrated on the face and extremities rather than on the trunk. It affects the face (in 95% of cases), and palms of the hands and soles of the feet (in 75% of cases). Also affected are oral mucous membranes (in 70% of cases), genitalia (30%), and conjunctivae (20%), as well as the cornea. The rash evolves sequentially from macules (lesions with a flat base) to papules (slightly raised firm lesions), vesicles (lesions filled with clear fluid), pustules (lesions filled with yellowish fluid), and crusts which dry up and fall off. The number of lesions varies from a few to several thousand. In severe cases, lesions can coalesce until large sections of skin slough off.
Treatment and Vaccine for Monkeypox Today
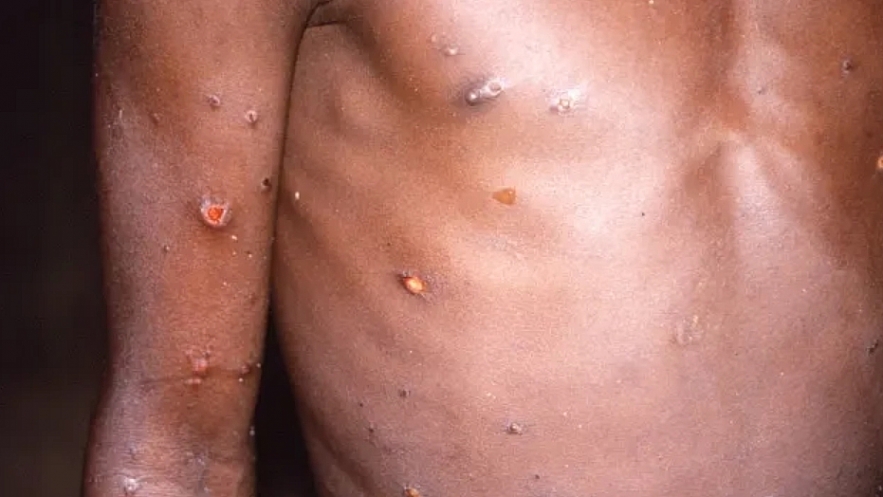 |
| Treatment and Vaccine for Monkeypox: An image created during an investigation into an outbreak of monkeypox, which took place in the Democratic Republic of the Congo, 1996 to 1997, shows the arms and torso of a patient with skin lesions due to monkeypox |
Currently, no treatment is available for monkeypox. Existing treatments for the disease were originally approved as a defense in case of a biological attack. The smallpox virus belongs to the orthopoxvirus family and shares significant similarities with an old enemy of humankind: smallpox.
Luckily, compared to smallpox, monkeypox is less deadly—between 1% and 3% of patients die from it, compared to smallpox’s 30% mortality.
Smallpox vaccine has been reported to reduce the risk of monkeypox among previously vaccinated persons in Africa. CDC is assessing the potential role of postexposure use of smallpox vaccine as well as therapeutic use of the antiviral drug cidofovir.
The two viruses are similar enough that treatments developed against smallpox can be used with monkeypox, too. And while there aren’t specific treatments for monkeypox—an existing disease that has affected thousands of people in several African countries since the 1970s—there are many available for smallpox.
The latest drugs approved by the Food and Drugs Administration (FDA) to treat smallpox are Tpoxx (generic name: tecovirimat), made by Siga Technologies, and Tembexa (generic name: brincidofovir), which Emergent Biosolutions just acquired from its developer Chimerix for $325 million. Both drugs are antivirals, taken orally or as an injection. There is also a smallpox vaccine, made by Bavarian Nordic, and another by Tonix Pharmaceutical in the pipeline.
Vaccines are available to control monkeypox outbreaks
While there are no retroactive treatments proved to cure monkeypox infections, there are a number of vaccinations that can prevent the spread and make instances of infection less severe. The Centers for Disease Control and Prevention advises that the smallpox vaccination, cidofovir, ST-246, and vaccinia immune globulin (VIG) can all be used to tackle a monkeypox outbreak.
In the United States the Jynneos vaccine, also known as Imvamune or Imvanex, has been licensed for the prevention of monkeypox. The monkeypox virus is closely related to smallpox so, despite initially being a smallpox vaccine, the Jynneos shot can protect recipients from monkeypox.
Data from recipients in Africa found that smallpox vaccines are at least 85% effective in preventing monkeypox infection. There is also evidence that vaccination after exposure to monkeypox may prevent a serious infection.
Use Smallpox Treatments for Monkeypox
That is a lot of options to treat a disease that was declared eradicated in 1980. But these vaccines and antivirals were not developed to cure existing illnesses. They exist in case someone decides to bring back smallpox (also known as variola virus) as a weapon.
While bioterrorism is a serious threat, there is something paradoxical about European countries having to order smallpox treatments from the US in order to treat monkeypox, a disease to which rich countries hadn’t given any thought since the first official case in 1970. But like the spread of covid, the recent monkeypox flare-ups show viruses heed no borders. “Saying ‘no one is OK if we are all not OK’ is not just a punchline, but a truth inherent to the principle of global health,” says Nadia Sam-Agudu, a pediatrics professor at University of Maryland’s Institute of Human Virology.
| US stocks up on monkeypox vaccines With confirmed case of monkeypox recorded in the US, health authorities are taking no chances and have ordered millions of doses of the Jynneos vaccine. The federal government has entered into an agreement to buy $119 million worth of the vaccination, produced by biotechnology company Bavarian Nordic. However the government also has a significant pre-existing order with Bavarian Nordic, made and invoiced in the past. The US will convert some of the previous orders into freeze-dried versions which can be kept for a longer amount of time. In total the government is tied in to $299 million of purchases from the pharmaceutical company, which is expected to provide 13 million doses of the smallpox/monkeypox vaccine. |
How do you prevent monkeypox virus?
A smallpox vaccine can provide protection against monkeypox, but its use is currently limited to people who work in a lab with the variola (smallpox) virus. Prevention depends on decreasing human contact with infected animals and limiting person-to-person spread. You can prevent monkeypox virus by:
⇒ Avoiding contact with infected animals (especially sick or dead animals).
⇒ Avoiding contact with bedding and other materials contaminated with the virus.
⇒ Washing your hands with soap and water after coming into contact with an infected animal.
⇒ Thoroughly cooking all foods that contain animal meat or parts.
⇒ Avoiding contact with people who may be infected with the virus.
⇒ Using personal protective equipment (PPE) when caring for people infected with the virus.
Raising awareness of risk factors and educating people about the measures they can take to reduce exposure to the virus is the main prevention strategy for monkeypox. Scientific studies are now underway to assess the feasibility and appropriateness of vaccination for the prevention and control of monkeypox. Some countries have, or are developing, policies to offer vaccine to persons who may be at risk such as laboratory personnel, rapid response teams and health workers.
Reducing the risk of human-to-human transmission
Surveillance and rapid identification of new cases is critical for outbreak containment. During human monkeypox outbreaks, close contact with infected persons is the most significant risk factor for monkeypox virus infection. Health workers and household members are at a greater risk of infection. Health workers caring for patients with suspected or confirmed monkeypox virus infection, or handling specimens from them, should implement standard infection control precautions. If possible, persons previously vaccinated against smallpox should be selected to care for the patient.
Samples taken from people and animals with suspected monkeypox virus infection should be handled by trained staff working in suitably equipped laboratories. Patient specimens must be safely prepared for transport with triple packaging in accordance with WHO guidance for transport of infectious substances.
The identification in May 2022 of clusters of monkeypox cases in several non-endemic countries with no direct travel links to an endemic area is atypical. Further investigations are underway to determine the likely source of infection and limit further onward spread. As the source of this outbreak is being investigated, it is important to look at all possible modes of transmission in order to safeguard public health.
Reducing the risk of zoonotic transmission
Over time, most human infections have resulted from a primary, animal-to-human transmission. Unprotected contact with wild animals, especially those that are sick or dead, including their meat, blood and other parts must be avoided. Additionally, all foods containing animal meat or parts must be thoroughly cooked before eating.
Preventing monkeypox through restrictions on animal trade
Some countries have put in place regulations restricting importation of rodents and non-human primates. Captive animals that are potentially infected with monkeypox should be isolated from other animals and placed into immediate quarantine. Any animals that might have come into contact with an infected animal should be quarantined, handled with standard precautions and observed for monkeypox symptoms for 30 days.
Q&A Monkeypox
What is the cause of monkeypox?
Monkeypox is caused by Monkeypox virus, which belongs to the orthopoxvirus group of viruses. Other members of this group of viruses that cause infections in humans include variola (smallpox), vaccinia (used for smallpox vaccine), and cowpox viruses.
What are the clinical features of monkeypox?
In humans, monkeypox is similar to smallpox, except that enlargement of lymph nodes (lymphadenopathy) is associated with monkeypox. About 12 days after exposure, the illness begins with fever, headache, muscle aches, backache, swollen lymph nodes, a general feeling of discomfort, and exhaustion. Within 1 to 3 days (sometimes longer) after the appearance of fever, the patient develops a papular rash (i.e., raised bumps), often first on the face but sometimes initially on other parts of the body. The lesions usually develop through several stages before crusting and falling off.
How long does monkeypox last?
The illness typically lasts for 2 to 4 weeks.
Is monkeypox fatal?
Studies of human monkeypox in rural central and west Africa - where people live in remote areas and are medically underserved - have reported case-fatality ratios of as high as 10%.
How do people get monkeypox?
Monkeypox is spread when you come into contact with an animal or a person infected with the virus. Animal-to-person transmission occurs through broken skin, like from bites or scratches, or through direct contact with an infected animal’s blood, bodily fluids or pox lesions.
Monkeypox can spread from person to person as well, but it’s less common. Person-to-person spread (transmission) occurs when you come in contact with virus particles from another person. When an infected person coughs or sneezes, the virus can be transmitted through airborne droplets. It requires prolonged face-to-face contact, but you can then breathe in these tiny droplets from someone else (respiratory droplets), or get them in your eyes or nose. You can also get it directly from touching the lesions on an infected person.
You can also get monkeypox by coming into direct or indirect contact with materials contaminated with the virus. These materials can include clothing, bedding and other linens used by an infected person or animal.
How is monkeypox diagnosed?
Because monkeypox is so rare, your healthcare provider may first suspect other rash illnesses, such as measles, chickenpox or even smallpox. However, swollen lymph nodes distinguish monkeypox from other poxes.
To diagnose monkeypox, your healthcare provider takes a tissue sample that is looked at using a microscope. You may also need to give a blood sample to check for the monkeypox virus or antibodies your immune system makes to it.
Have monkeypox cases been reported in the U.S. before?
Yes. Last year, two separate cases were confirmed in Texas and Maryland in people who had returned from traveling to Nigeria.
And in 2003, an outbreak occurred in six states — Illinois, Indiana, Kansas, Missouri, Ohio and Wisconsin — when 47 people were infected with monkeypox after coming into contact with pet prairie dogs. The pets had previously been housed near small mammals imported from Ghana that were infected with the virus.
Could the virus become more transmissible and thus more of a global threat?
Scientists are keeping a close eye on the virus and outbreaks that occur — especially if the virus appears to change its route of transmission, as may be happening in the current outbreak.
Many scientists didn't think SARS-CoV-2, the coronavirus that causes the disease COVID-19, would mutate to become more contagious, but that's exactly what has happened in the past two years. SARS-CoV-2 evolved from a virus just about as contagious as the flu virus into one that's almost as contagious as the far more transmissible chickenpox virus.
And indeed, this new outbreak in Europe may be a sign that the virus has changed — even if just a bit — and may be increasing its ability to spread among people.
How common is monkeypox?
Monkeypox is rare. But the number of cases in Africa has been increasing. Smallpox and monkeypox are caused by similar viruses, so when people were vaccinated against smallpox it also protected them from getting monkeypox. Since smallpox is no longer a disease and people are no longer vaccinated against it, they don’t have that protection against monkeypox.
Where else is monkeypox found?
Monkeypox has mostly been seen in the Democratic Republic of the Congo. However, it’s occasionally found in other countries, including the United States. In the spring of 2003, the first outbreak of monkeypox outside of Africa occurred in the United States. A shipment of infected animals from Ghana was imported into Texas. The infected rodents spread the virus to pet prairie dogs, which then infected 47 people in the Midwest. In the summer of 2021, a case of monkeypox was found in a U.S. resident who had traveled from Nigeria to the United States.
Who does monkeypox affect?
Anyone can get monkeypox. However, it’s more common in children. Of cases in Africa, 90% were among children under 15 years old.
 14 Most Common Andrological Diseases That Every Man Should Know 14 Most Common Andrological Diseases That Every Man Should Know Learning about andrological diseases is essential for men to detect and treat promptly, helping to limit complications later, according to andrologists. |
 What is Norovirus: Symptoms and best treatment What is Norovirus: Symptoms and best treatment There are several causes of food poisoning or “stomach flu.” Norovirus is a major one. It’s highly contagious. It often spreads through contaminated food, water, ... |
 Top 15 Most Common Infectious Diseases in America (part 2) Top 15 Most Common Infectious Diseases in America (part 2) People in the United States continue to get diseases that are vaccine-preventable. |
 Top 15 Most Common Infectious Diseases in America (Part 1) Top 15 Most Common Infectious Diseases in America (Part 1) People in the United States continue to get diseases that are vaccine-preventable. The list below aims to provide basic information about the top 15 |